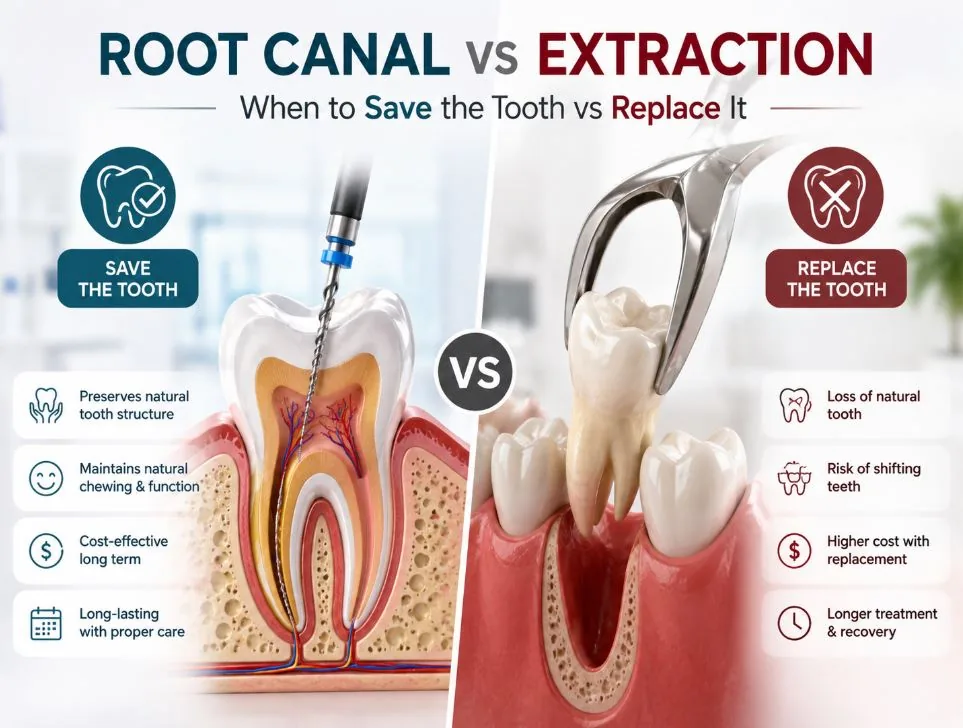
When a tooth has deep decay, a failed restoration, or recurring infection, you'll often face a choice: a root canal to save it, or an extraction with an implant or bridge to replace it. Both are evidence-supported procedures with high long-term success rates. Neither is universally "better." The right answer depends on what's actually salvageable, what the long-term economics look like, and what your specific clinical situation supports. This guide walks through that decision framework honestly, with citations to peer-reviewed survival data for both paths.
Most patients arrive at this decision under time pressure — a tooth is hurting, the dentist needs to act, and the consultation is rushed. That's exactly when a clear framework matters most. The wrong call in either direction is expensive: an unnecessary extraction permanently removes natural tooth structure that no implant fully replaces; an unnecessary root canal on a fractured or non-restorable tooth wastes time and money before you end up extracting it anyway. Knowing the indicators in advance lets you steer the consultation toward the right answer rather than the fastest one.
The Basic Tradeoff
Saving a tooth via root canal preserves the natural structure — the actual enamel, dentin, periodontal ligament, and sensory feedback that the tooth has had since you grew it. Modern endodontics achieves long-term success in 86-98% of cases when done to current standards and properly restored afterward. The treated tooth integrates with the bite, the bone, and the gum the way a natural tooth always has.
Replacing a tooth with an implant means surgically extracting the damaged tooth, allowing the bone to heal (or grafting if needed), placing a titanium implant body, waiting 3-6 months for osseointegration, and then placing an abutment and crown. Modern implants achieve approximately 95% 10-year survival rates per peer-reviewed implant cohort studies. They function well, they look natural, and they're a definitive solution for teeth that genuinely cannot be saved.
So the question isn't "which procedure is better." It's "which procedure fits this specific tooth, this specific situation, and these specific outcomes you care about." The answer almost always lies in the clinical particulars of the tooth in question.
When Root Canal Is the Right Call
Root canal is the right first option when the tooth still has the structural foundation to support a crown afterward and the failure mode is treatable through endodontic intervention.
When Extraction + Implant Is the Right Call
Extraction is the right call when the tooth genuinely cannot be reliably saved, when retreatment options have already failed, or when the strategic value of the tooth doesn't justify the preservation effort.
The Cost Comparison Honestly
Cost is not the only factor in this decision, but it is a real one. Here's the realistic 2026 U.S. all-in cost for each path:
| Path | Component | Typical Cost |
|---|---|---|
| Root Canal + Crown | Root canal (molar) | $1,200 – $2,400 |
| Crown | $1,000 – $2,500 | |
| Total | $2,200 – $4,900 | |
| Extraction + Implant + Crown | Extraction | $200 – $500 |
| Bone graft (if needed) | $400 – $1,500 | |
| Implant body | $1,500 – $3,000 | |
| Abutment + crown | $1,500 – $3,000 | |
| Total | $3,600 – $8,000+ |
Insurance coverage differs between the two paths. Root canals are typically covered as "major" procedures at 50-80% up to the annual maximum (~$1,500-2,000). Implants are often partially covered or excluded entirely depending on the plan. The crown component on the implant is usually covered. Net out-of-pocket for the implant path tends to be meaningfully higher even after insurance.
The Timeline Comparison
Time matters when you're trying to plan around work, travel, family obligations, or simply just wanting to be done with a dental issue.
| Path | Visits | Total Time to Final Function |
|---|---|---|
| Root canal + crown (no complications) | 2-3 visits | 2-4 weeks |
| Root canal + crown (with retreatment) | 3-5 visits | 1-3 months |
| Extraction + implant (no graft) | 3-4 visits | 4-6 months |
| Extraction + implant + bone graft | 4-5 visits | 6-9 months |
The timeline gap is real. If you have a wedding next month, a major work event, or simply hate sustained dental projects, the root canal path is meaningfully faster from "hurts now" to "fully functional again."
The Success Rate Comparison
Both paths have high success rates. Long-term outcome data is published in peer-reviewed dental literature for both, and the numbers are honest:
| Procedure | Long-Term Survival/Success Rate |
|---|---|
| Initial root canal (vital pulp) | ~95-98% at 5-10 years |
| Initial root canal (with periapical lesion) | ~80-90% at 5-10 years |
| Endodontic retreatment | ~70-85% at 5-10 years |
| Single-tooth implant | ~95% at 10 years |
| Implant in grafted site | ~92-95% at 10 years |
Both procedures can fail. The failure modes differ — root-canaled teeth fail through reinfection, vertical fractures, or restoration breakdown; implants fail through peri-implantitis, integration failure, or mechanical complications. Neither is "always" anything. Choose based on which procedure fits your specific clinical situation, not on which has the higher topline success number.
The Biological Argument for Tooth Preservation
Natural teeth have biological features that implants don't replicate. None of these are catastrophic on the implant side, but they're real advantages of saving the tooth when it's saveable.
Natural bone preservation — chewing forces transmitted through the periodontal ligament stimulate the surrounding alveolar bone. This is why bone resorption follows extraction. Implants preserve bone too (they're loaded with chewing forces) but the mechanism and biological pattern is different.
Micro-movement under load — natural teeth move slightly under chewing forces (~25-100 microns), which distributes stress and prevents fracture. Implants are rigidly osseointegrated and don't move, which means stress concentrates at the implant body and crown junction. This is part of why implant crowns sometimes fracture or screws loosen over years.
No surgical placement of foreign material — implants are titanium fixtures placed into the jawbone via a surgical procedure with normal surgical risks. Root canals don't introduce foreign material into the jawbone.
None of these are reasons to save an unsalvageable tooth. They're reasons not to extract a salvageable tooth without considering whether saving it is the better long-term outcome.
The Case for Extraction (When It's Warranted)
The biological-preservation argument can be misused — it can push patients into futile retreatments of teeth that should have been extracted months ago. Modern implants are excellent prostheses with decades of outcome data behind them. When the tooth genuinely cannot be saved, an extraction and implant is the right path, and the outcome is generally very good.
The key word is "genuinely." Don't accept a same-day extraction recommendation on a tooth that hasn't been properly evaluated for endodontic salvage. Don't accept a same-day "save it at any cost" recommendation on a tooth that's clearly fractured and unsalvageable. Get the imaging, get the second opinion if anything feels unclear, and make the decision based on the actual structural and biological condition of the tooth rather than on either an ideological preference for preservation or a financial preference for the more profitable procedure.
Five Questions to Ask in This Decision
Red Flags in This Decision
"All root canals fail eventually" framing — false. Modern root canal long-term success is 86-98% per peer-reviewed cohort studies. The implant success rate is ~95% at 10 years. Both procedures have failures; neither has "always."
Heavy pressure toward whichever procedure the practice does most volume of — implants are typically more profitable per case than root canals. Endodontic specialists, conversely, may steer toward root canal even on poorly-prognosis teeth. The bias can run in either direction. The right answer is the one supported by your specific clinical situation.
Recommendations citing the focal-infection-theory pseudoscience — "extract the tooth because root canals are toxic" is a recommendation rooted in 1920s science discredited by the 1950s. The American Dental Association and American Association of Endodontists have published explicit position papers refuting this claim. If a provider recommends extraction on this basis, find a different provider.
No CBCT imaging on a complex case — CBCT meaningfully changes diagnostic accuracy on root fracture, canal anatomy, and bone support evaluation. A provider working from 2D X-rays alone on a structurally questionable tooth is operating with less information than the case warrants.
Putting It Together
The most important thing to know going into this decision is that there is no universal right answer. There is only the right answer for your specific tooth, in your specific clinical situation, with your specific priorities. The framework above gives you the actual indicators that should drive the decision — not which procedure your dentist personally prefers, not which is the "newer" or "trendier" option, not which is the most profitable for the practice, and not which is the cheapest in the moment.
Get the imaging. Ask the five questions. Get a second opinion if the recommendation feels rushed or one-sided. The tooth you keep today is the one you don't have to replace tomorrow — but the tooth that genuinely can't be saved isn't worth the months of futile treatment when a definitive replacement is the better long-term answer. Decide on the merits, not on the framing.
For the broader context on root canals — what they actually involve, the peer-reviewed evidence on safety, and the spectrum of cases they handle — see the main root canal guide. For implant-side cost realities, the affordable dental implants guide covers what real implant pricing looks like. If you're already in the failed-root-canal scenario, the retreatment options guide covers the decisions before extraction is on the table at all.
Find a Provider for an Honest Second Opinion
Browse Smyleee's curated directory of vetted endodontists, general dentists, and oral surgeons across the U.S. — credentials verified, transparent pricing, both root canal and implant providers.
Sources & References
- American Association of Endodontists — Position Statements (Treatment Outcomes; Endodontic Treatment Is Safe)
- American Board of Endodontics — Board Certification Standards
- American Dental Association — Endodontics Oral Health Topic
- Cochrane Reviews — Endodontic Treatment Outcome Systematic Reviews
- Journal of Endodontics — Long-Term Tooth Survival Studies
- American Academy of Implant Dentistry — Implant Survival Outcome Data
- Academy of Osseointegration — Peer-Reviewed Implant Outcomes Research
- MetLife Oral Fitness Library — Procedure Cost References
- GoodRx — Dental Procedure Cost Guides
- CareCredit — Dental Procedure Financing
- American Dental Association MouthHealthy — Patient Resources
- U.S. Food and Drug Administration — Dental Device Safety Guidance
- IRS Publication 502 — Medical and Dental Expenses (HSA / FSA Eligibility)